Naval Specialty Medical Center Program Team
Clinical reports and pathologic anatomic findings shown, progressive hypoxemia is the main cause of deterioration in patients with COVID-19.”The mortality rate of critical patients in WuHan is close to 60%, and we are trying to solve the problem of hypoxia,” Zhong Nanshan said on 27 th Feb. HBOT is the strongest non-invasive oxygen therapy. In the early stage, 5 cases of severe and critical patients with COVID-19 a were clinically treated, which proved that the long-term excellent clinical effect of using HBOT in treating hypoxia was also applicable to COVID-19 patients. The effect of HBOT is better than breathing atmospheric high flow oxygen and mechanical ventilation techniques. It is suggested that promote HBOT as an oxygen therapy treatment for critically ill patients with COVID-19, which is expected to significantly improve the treatment efficiency, reduce the medical pressure and the risk of infection, and decrease the mortality rate of critical patients. It has practical significance for further accelerating the overall victory of this epidemic, achieving the most effective treatment and realizing infection prevention control.
I. Evaluation of the effectiveness of HBOT in oxygen therapy for critical patients with COVID-19.
1) critical patients showed consistent response to HBOT oxygen therapy
___
Hyperbaric Chambers for sale on eBay
___
Zhong Yangling, the director of the Department of Hyperbaric Oxygen in Wuhan Yangtze River Shipping General Hospital, successfully carried out HBOT treatment in 5 patients with COVID-19 (2 critical and 3 severe), which got significant results. Case reports of the first patient have been published. 5 cases clinical analysis data shown:
a) Treatment effect of progressive hypoxemia in severe patients
-Rapid relief of hypoxic symptoms. 5 patients had obvious symptoms of progressive hypoxia before. After the first session of HBOT, symptoms such as dyspnea and chest pain are reduced. After the second session HBOT, the symptoms are basically relieved, and the respiratory rate decreases gradually, but the shortness of breath after the movement relieved slowly.
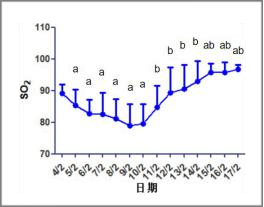
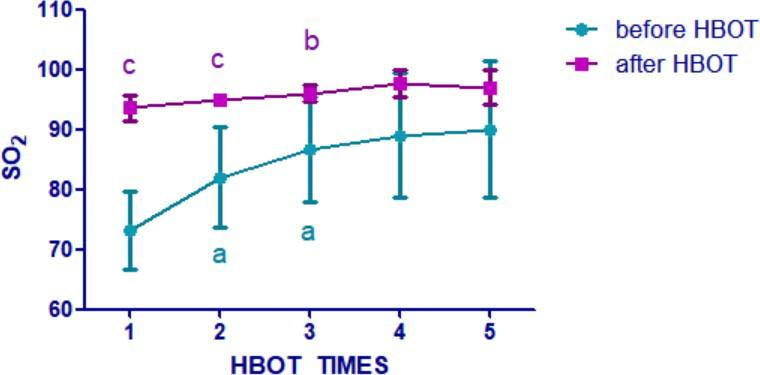
-Rapid correction of hypoxemia. Arterial blood gas analysis of 5 patients under the condition of breathing oxygen with oxygen mask (5~8L/min) before HBOT treatment showed PaO2 is 37, 65, 60, 78, and 68 mmHg, the trend of critical patients’ Blood oxygen saturation of artery blood of finger(SO2)was reversed immediately. Since the 5th day,SO2 was up to 95% in daily average(pic1). Compare with the patients’ body databefore they do the HBOT treatment,which be regard as the last day data, SO2 showed a significant upward trend day by day(2 left). After HBOT treatment, SO2 is higher than 93%, and every treatment solved the patient’s problem of total hypoxia. Arterial blood gas index recovered significantly(pic 2a).
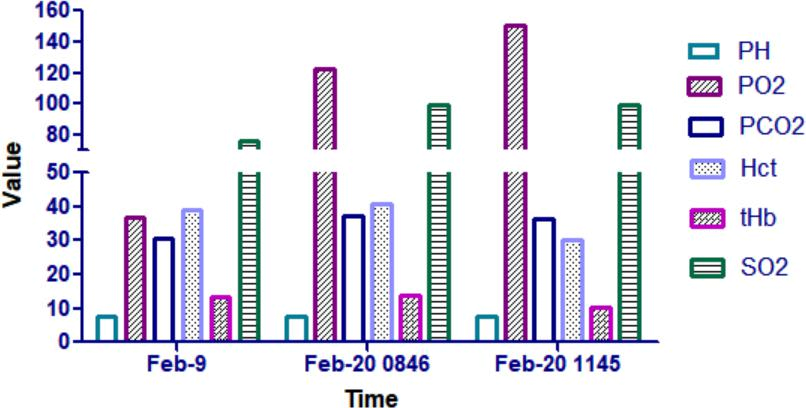
b) Comprehensive therapeutic effect of HBOT oxygen therapy on severe patients
– General condition reversal. In addition to the relief of hypoxic symptoms in all patients, the general state was significantly reversed. Gastrointestinal symptoms are reduced and appetite is restored. Headache disappeared and mental state improved.
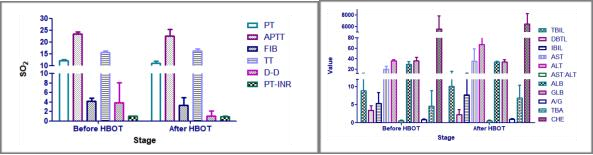
– Clinical objective indicators improved. Except the significant changes in artery blood of finger and Arterial blood gas, differential blood count, which respond to immune function recovered gradually, coagulation index of reactive peripheral circulation disorder improved, Indexes reflecting liver function and myocardial injury improved(pic3).
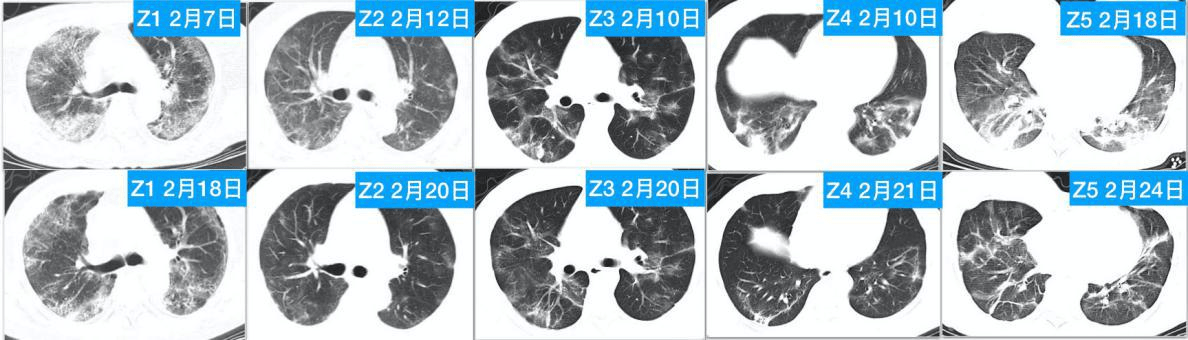
– Improved lung pathology. Re-examination of the lung CT after treatment showed that lung inflammation in all 5 patients was significantly improved(pic4).
2) The mechanism of HBOT oxygen therapy
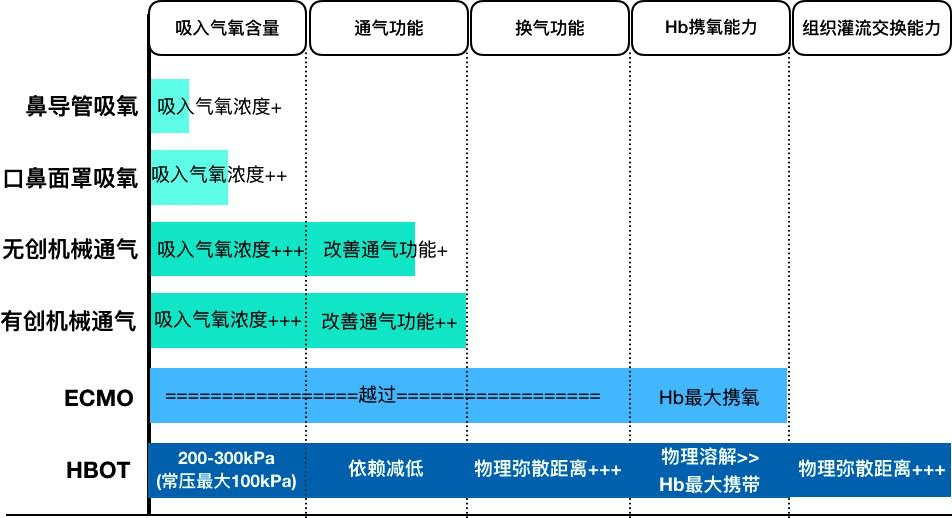
The difference between HBOT oxygen therapy and normal pressure oxygen therapy is, in general, the use of high pressure oxygen inhalation, which fully and substantially improves the efficiency of oxygen transport from the outside to the whole tissue cells. The mechanism of HBOT is to take advantage of the physical characteristics of gas, to increase the partial pressure of the oxygen in the environment through a large amplitude, and to reduce the demand for oxygen exchange and transportation in the body to achieve the best oxygen therapy effect. The mechanism of HBOT is shown in pic 5. The advantages compared with atmospheric pressure oxygen therapy technology are:
Firstly, more effectively than normal pressure oxygen inhalation to overcome lung tissue inflammation.
The diffusion rate and distance of high pressure oxygen are several times that of normal pressure oxygen, which overcome the gas exchange obstacle caused by the thickening of the lung tissue inflammation. And because of the higher solubility, the amount of oxygen dissolved in the blood is several times that of atmospheric oxygen, which also further overcomes the influence of the blood circulation gas ratio.
Secondly, it is more effective to increase oxygen partial pressure than to increase oxygenation index by mechanical ventilation.
In respiratory and critical care medicine, oxygen efficiency in clinical respiratory support uses oxygenation index (is the ratio of partial pressure of oxygen in the artery to partial pressure of oxygen in the inhaled gas [OI=PaO2/FiO2(air pressure /760)])) as the final evaluation index. With partial arterial oxygen pressure as the therapeutic target, the conversion formula[PaO2=OI × FiO2(air pressure /760)]. Mechanical ventilation technique is to improve PaO2 by increasing OI. The FiO2 of HBOT can be increased by 1.6~2.8 times. It can be predicted that PaO2 can be increased by 1.6~2.8 times with HBOT patients’ OI unchanged, which is the same as the effect of OI increased by 1.6~2.8 times. The effects of OI and treatment before treatment in 5 patients have been fully verified. In one case, HBOT was used to reverse hypoxia on the basis of no effect of noninvasive mechanical ventilation for 2 days. HBOT technology for patients with invasive mechanical ventilation is mature and has been routinely used in clinical HBOT. Therefore suggested that clinical selection principles are: (1) HBOT treatment is preferred when patients’ oxygenation index is significantly reduced and natural respiration is clear, and mechanical ventilation is not expected to increase oxygenation index by 1.5 times; (2) When the improvement of oxygenation index under mechanical ventilation is less than twice that of natural respiration, it is suggested to increase the daily HBOT treatment on the basis of mechanical ventilation.
Thirdly, more effective than ECMO in improving tissue cell oxygen uptake.
Although ECMO has surpassed the ventilation and gas exchange functions of the lungs, and can make Hb completely saturated, it is not as good as HBOT in tissue side oxygen supply. The dissolved oxygen in the blood has exceeded the amount carried by Hb, and the diffusion distance has been greatly increased, which can relatively overcome the peripheral circulation obstacles caused by pre-hypoxic damage or / and infectious inflammation, and improve the efficiency and absolute amount of tissue cells to obtain oxygen.
Fourthly, there is no serious interference of mechanical ventilation to the respiratory tract in natural breathing.
HBOT means that the patient is under high pressure. The common metaphor of the difference between breathing mode and atmospheric pressure is that breathing on the plateau is the same as breathing on the plain, which is natural breathing. Different from mechanical ventilation, it has a great effect on respiratory tract, need to be paid attention to and dealt with by doctors and nurses at all times. Otherwise, it is easy to have various complications such as airway injury.
Fifthly, there is no conflict with the current means of critical treatment, and the +HBOT mode has a clear role in improving the treatment effect.
COVID-19, in addition to antibodies and vaccines, there is no specific drug. All clinical treatment is basically symptomatic treatment and supportive treatment. HBOT is not the etiological treatment of COVID-19, it is the symptomatic treatment of hypoxia in patients with COVID-19, and it is a supplement to the existing oxygen treatment technology. In addition to HBOT once a day for 95-120 minutes, the patients also received the existing comprehensive treatment in ICU, including mechanical ventilation. In addition to HBOT, ICU clinicians are still responsible for the daily comprehensive treatment of the above-mentioned severe patients. There is no conflict in treatment technology. On the contrary, it can provide better support for other supportive treatments.
process of tissue and organ)
3) Clear indications of HBOT for the symptomatic treatment of hypoxia
Firstly, hypoxia is the first indication of HBOT.
HBOT is a routine oxygen therapy for clinical refractory hypoxia. HBOT has been widely used in the clinic for more than half a century since it was first used in the supportive treatment of thoracic surgery in 1956. In China, grade A hospitals are generally equipped with oxygen Chambers, and a large number of HBOT of various diseases are carried out on a daily basis, especially for carbon monoxide poisoning — a typical acute anoxia, which has become a key treatment measure. From the perspective of diseases, HBOT has a wide range of indications. As a routine application of oxygen therapy, the indication is essentially a “hypoxia”, that is, generalized and local stubborn hypoxia problem.
Secondly, the diagnosis of anoxia in severe patients with COVID-19 is clear.
The clinical manifestations of severe patients with hypoxia are prominent, the indication of hypoxemia is obvious, and the existence of hypoxia is obvious. In all the previous published clinical scientific literature on COVID-19, it is clear that the continuous and progressive development of hypoxemia is an important manifestation of disease deterioration. In the severe treatment of COVID-19, HBOT is used for the symptomatic treatment of anoxia correction with clear indications.
The therapeutic effect of 5 patients was very significant, and both the subjective and objective clinical indexes showed that the deterioration of hypoxia was interrupted immediately and then the whole body recovered gradually after the first HBOT. Such a consistent treatment response, according to the statistical law, cannot be explained by chance. The above mechanism demonstrated that the efficacy of HBOT in 5 patients was not accidental. The therapeutic effect of HBOT on hypoxia is a scientific summary of the effects of HBOT in the treatment of intractable and refractory hypoxia in various diseases over a long period of time. The relevant scientific papers, literature and works are endless. The superiority of HBOT in solving severe hypoxia in patients with COVID-19 is clearly scientific. Unlike the newly developed treatment stage or the efficacy of medicine is still in the scientific hypothesis stage, HBOT don’t need clinical trial verification and other methods of oxygen therapy that have been used clinically, such as mechanical ventilation or
ECMO, it can be reasonably used.
In summary, the use of HBOT can provide clear clinical benefits for the pathophysiological problems encountered in the treatment of hypoxia in severe critical diseases. HBOT can be used to treat severe hypoxia in patients with COVID-19, which can more effectively and comprehensively solve the problem of hypoxemia than normal pressure oxygen therapy (high flow oxygen inhalation, mechanical ventilation), make deep tissue hypoxia fully corrected and greatly relieve systemic hypoxic inflammation, and also has practical clinical significance for the effects of other treatment methods (such as medicine supportive treatment).
II. Safety of HBOT for oxygen therapy in severe patients with COVID-19
HBOT has been standardized and widely used clinically for nearly a century. Its essential medical safety is not repeated here. The focus is on disease prevention and control (CDC) risks posed by Class A infectious diseases. HBOT treatment requires special equipment and procedures, and patients need to be transferred back and forth from the ward to the hyperbaric oxygen chamber. The transfer process is in an atmospheric environment, and there are mature CDC measures without insurmountable technical problems. Wuhan Changjiang General Hospital has already formed a practicable method, which can be further improved, and it will not be repeated here. This article focuses on the treatment process of HBOT in the oxygen cabin and the risk of CDC in the hyperbaric oxygen department.
1) . The risk of pathogenic microorganism infection in cabin is not higher than the ward
Firstly, the risk of performing CDC in the hyperbaric oxygen chamber is the same as the risk of CDC in the infection ward.
The difference between the micro-environment of the hyperbaric oxygen chamber and the micro-environment of the infection ward is the radon pressure.It is same as the difference between the plateau and sea level. The medical staff is exposed to the oxygen chamber micro-environment under a high pressure, the surface intensity of pressure is equal, and the pressure difference cannot be felt. Protective equipment also does not suffer from “compressive” deformation. The requirements for the infection control of the hospital in plateau area are not different from those in the plain area. There are no clear differences in CDC requirements for different environmental pressures. The process of medical treatment in the hyperbaric cabin did not significantly increase the risk of CDC compared with the same operation in the infection ward.
Secondly, the hyperbaric oxygen cabin is a completely new wind environment.
In the HBOT process, “ventilation” measures are usually adopted. The pressure valve and the pressure relief valve are opened at the same time.When the amount of air input is equal to the amount of air output, the intensity of pressure in the cabin is guaranteed to be constant, and the air purge inside cabin is continuously updated. The air inlet port and output port are located on the opposite sides of the cabin. Under continuous ventilation, the air flow in the cabin is generally unidirectional,similar to a laminar flow operating room. The pressure of the air in the pipeline decreases gradually from the source to the exhaust port. There is no back flow of gas under the pressure gradient. The air sources are filtered, pressurized, and depressurized by an oil-free air compressor advanced purification device to ensure clean air sources.
Thirdly, air breathed by doctors and patients is relatively separated inside the cabin.
The patient used a mask of the Bulding in breathing system (BIBS) to breathe pure oxygen after entering the cabin. The exhaled gas of the patient mainly exists in the oxygen exhaust line and flows unidirectionally outward. Medical staff breathes air in the cabin, basically does not cross the gas that the patient breathe. This is better than the infection ward.
Medical staff pressurize independently. During the pressurization process, the pressure on the body side of the protective equipment is low, and the air in the cabin may enter the body side of the protective equipment as the pressure increases. The hyperbaric oxygen chamber is provided with a transition cabin (small cabin). The medical staff use independent cabin to pressurize to avoid the possibility that a large amount of air from the treatment cabin where the patient is regarded as a contaminated area enters the body side of the protective equipment. The decompression process is the opposite, so there is no risk of CDC.
Fourthly, Infection ward CDC measures are used in the hyperbaric oxygen chamber and no additional evaluation is required.
The hyperbaric oxygen chamber is managed as a ward for patients with new coronavirus. Disinfection process is performed under normal pressure, and the disinfection technology method and effect are the same. The pressurization process is with “full fresh air systems”, the air that doctors and patients breathe is relatively independent, and the possible gas pollution is less than that of infected wards. In addition, the CDC requirements for infection wards are applicable to infection-control management after the pressure in the hyperbaric chamber is relatively constant.
2). Hyperbaric Oxygen Department’s measures to control infection have been initially formed and practical
The Hyperbaric Oxygen Department is an area for the treatment of infected patients. There are clear rules and regulations for the setting of the ward isolation area and personnel protection under normal pressure, which can a reference. It has also formed a set of effective practices, which will not be repeated here. The focus of controlling infection is to purify and sterilize the exhaust gas from the BIBS system oxygen outlet and chamber decompression outlet of the patient’s breathing. In this regard, no products were found at home or abroad for hyperbaric chamber exhaust gas purification and disinfection. We first adopted strict control measures in the area of the exhaust port to avoid the possible impact of the patient’s exhaled gas on the outside activities in the effective area. At the same time, non-standard disinfection measures were temporarily adopted, and the exhaust gas was filtered by the disinfectant solution to further prevent the pollution of the exhaust gas to the surrounding environment and cause the virus to spread. At present, the hyperbaric chamber supplier has purchased the medical gas purification equipment certified by the relevant national authorities for modification. After installation, it can meet the national standards.
To sum up, the hyperbaric oxygen chamber is a closed gas management system with unidirectional air flow, full fresh air systems, and separate air pipelines for medical staff and patients to breathe. There are no insurmountable technical obstacles to the treatment of HBOT for CDC. Hyperbaric Oxygen Department of Wuhan Changjiang Shipping General Hospital has established a complete infection control procedures and measures for HBOT treatment of patients with new coronavirus, and has passed the evaluation of the infection control department. The HBOT treatment for patients with severe disease has been carried out more than 20 times in the early stage, and none medical was infected. In general, the risk of infection in the HBOT chamber is not as high as the ward. Early intervention of HBOT can reduce the use of mechanical ventilation and accelerate the cure of critically ill patients, and further reduce the risk of infection for medical staff.
III. Feasibility Evaluation of HBOT Oxygen Therapy at Huoshenshan Hospital for COVID-19
Huoshenshan Hospital will be the last line of defense for COVID-19. The above discussion shows that it is obvious that HBOT can be used for oxygen therapy in patients with COVID-19 if it can exert its clinical significance. But Huoshenshan hospitals are not equipped with HBOT equipment, which is the biggest problem with HBOT. Given that the treatment of hypoxia is a key and difficult point in the current severe treatment, it is of practical significance to strive for HBOT oxygen therapy in Vulcan Hospital. The following preliminary suggestions are made on the feasibility and progress of Huoshenshan Hospital’s existing treatment + HBOT.
Step1. Portable high-pressure oxygen equipment is used in a small area, and a basic treatment process adapted to the actual situation of Huoshenshan Hospital is formed.
In addition to the hyperbaric oxygen chamber, the equipment that can inhale oxygen at high pressure also has a diving chamber for treating decompression sickness. The military-equipped electric diving pressurized chamber and portable High-pressure chamber can also treat decompression sickness, and can be performed automatically in a good oxygen environment in a short time(120min) without the help of medical staff.
A military university in Wuhan is equipped with a mobile diving chamber (for two people) and a portable hyperbaric oxygen chamber. Therefore, hyperbaric oxygen therapy can be performed in the open area of the hospital. This part of the area is controlled according to the contaminated area and meets the CDC. It is recommended that the equipment and operator be transferred to Huoshenshan Hospital together to try HBOT treatment for 5 critically ill patients with similar conditions. Basic treatment procedures and CDC procedures include:
(1) HBOT treatment: 1.6ATA / 120 minutes, continuous oxygen inhalation. It is expected to achieve an oxygen therapy effect of 1.6 times the oxygenation index, which is superior to mechanical ventilation, the reasonable use of atmospheric oxygen, and the overall therapeutic effect is significant.
(2) CDC process of HBOT treatment: The CDC process of hyperbaric oxygen therapy in Wuhan Changjiang Shipping General Hospital has been proven to be feasible in time, and can be optimized and adjusted according to the actual layout of Huoshenshan Hospital.
(3) HBOT emergency treatment plan: HBOT uses 1.6ATA, diving depth is about 6 meters, no decompression is needed. Once the patient’s condition has changed, it can be removed from the compression chamber within 3 minutes. What you need to do is prepare first aid at atmospheric pressure next to the oxygen chamber, and then take the patient back to the ICU ward.
Step2. Concentrate portable hyperbaric oxygen equipment inside and outside the army to popularize HBOT oxygen therapy as much as possible
After researching the mobile high-pressure system capable of treating decompression sickness and combining the number of military equipment, preliminary estimates are that it can increase 144 times/day HBOT.
Step3. Hyperbaric Oxygen Chamber Construction at Huoshenshan Hospital Simultaneously Started
Construction of a new hyperbaric oxygen chamber system started at Huoshenshan Hospital. After investigation, the supplier of hyperbaric oxygen equipment of Wuhan Changjiang Shipping General Hospital can complete the installation and commissioning and put it into use within 15 days. HBOT oxygen therapy for tracheal intubation mechanical ventilation patients can be further developed and combined with portable hyperbaric oxygen equipment, the overall effect will be very significant.
Conclusion
In general, HBOT oxygen therapy has clear indications for patients with COVID-19, with obvious effects and no obvious uncontrollable safety risks. Control measures and procedures have been developed to meet the course of treatment for patients with Class A infectious diseases. The risk of infection by medical staff is not greater than that of infected wards. HBOT oxygen therapy is widely used, and some hospitals are also equipped with a hyperbaric oxygen chamber. Therefore, we strongly recommend including HBOT in the treatment of COVID-19 in order to provide the treating physician with more effective oxygen therapy. Huoshenshan Hospital, as the last line of defense for new serious treatment, is gradually exploring and developing large-scale HBOT oxygen therapy, which is expected to significantly improve treatment efficiency, reduce medical and infection pressure and reduce mortality.